 |
 |
 |
 |
Biomechanical Problems presenting in Pre-adolescence and Adolescence
Adolescence is a period of rapid musculoskeletal and physiological growth. Musculoskeletal injuries that are not correctly diagnosed and managed as a pediatric injury can be a significant source of disability in adulthood.
In Sweden, already in preadolescence, individuals involved with sports are faced with deciding to play 100% on their team or quit. The sporting culture has moved away from playing sports by season, which reduces the risk for injury while simultaneously positively impacting the nervous system. During the growth spurt the skeleton is actually weaker and more susceptible to injury: musculoskeletal injuries in children. An increase in training frequency and intensity during this period is associated with musculoskeletal injury including spinal injuries. These injuries are commonly misunderstood and poorly managed both because of the culture of sports and the lack of understanding of pediatric anatomy and physiology. Read more here.
Neck pain and headache are a common problem in pre-teens and teens. Children that have had some history of a head, mouth, nose or neck injury, even as a young child, are prone to biomechanical problems in the neck. These can be a source of neck pain and headache that do not respond to medication or traditional exercises. These can present separately or they occur together. Vision problems must always be ruled out in headaches as a first step. Headaches can be associated with stressful situations, genetics or both. Migraine headaches have a genetic component and can be true for tension headaches as well. Excessive screen time particularly with suboptimal ergonomics can lead to eye strain, headache and neck pain. Read more here.
Spinal asymmetry becomes evident in pre-teens and may or may not progress in adolescence. There are different reasons why children develop spinal asymmetry. These cause suboptimal biomechanics which can become symptomatic when strained. Proper assessment and management is critical for long term well-being. Vitamin D deficiency is not uncommonly associated with different skeletal asymmetries. Children with leg length discrepancy have an asymmetry while standing, which is not evident in positions where the leg length does not contribute to weight bearing. This is easily diagnosed during the physical examination. A scoliosis is not dependent on a weight bearing position and more often occurs among girls. Read more here.
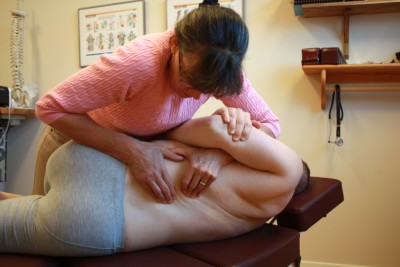
Pediatric Chiropractor As Biomechanical Specialist
Having your childs’ biomechanics assessed is important in helping them avoid spinal pain in the adult years. Research has shown that debilitating pain in adulthood has its’ roots in childhood/adolescence. This is true for low back pain, neck pain and headache. An examination focuses on posture, stance, leg length, foot type, asymmetries and curvatures in the spine. We assess the functioning of the spine and different joints. We evaluate neuromuscular integrity and can examine all the joints of the body (except the inner ear…). An important focus is assessing the kinetic chain. The kinetic chain describes how the action (or dysfunction) of the foot, ankle, knee and hip all have an impact on the functioning of the pelvis and low back. Understanding the scope of the problem, addressing dysfunction of the joints and musculature involved sets the ground work for a rehabilitative program for stability in the long term.
We make recommendations which can include self-help and instructions in appropriate exercises.
What are common problems that we treat in our office?
We start at the feet. We evaluate the function of the feet and by improving the mobility of all the small joints many problems causing discomfort can be addressed. Some causes of pain or discomfort actually originate in the low back, so we are always considering this as a possibility of why a patient has foot pain. Some of the different types of problems are heel spur (hälsporre), Achilles tendonitis, Morton’s neuroma, hallux rigidus, hallux valgus, plantar fasciitis among others. In some cases we tape the foot for a period of time to address instability. Our role is to improve function by mobilizing or manipulating different parts of the foot. Once function is improved, exercises to stabilize the foot and appropriate foot wear are recommended.
The knee is a hinge joint. When function is impaired this leads to instability and strains primarily the surrounding joints. In some patients knee pain reflects a primary problem in the hip and must be differentiated. We have these important skills in differential diagnosis. Understanding the origin of the problem is the first step in the assessment of the patient. Only then can adequate treatment be performed and proper rehabilitation recommended. The goal with treatment is to restore normal function in the joint and to recommend exercises to stabilize the joint. In some cases a brace to stabilize the knee is needed.
The hip joint is a ball and socket joint that is part of the pelvis, it is a very stable. Reduced mobility in this joint directly strains the joints of the pelvis and lumbar spine. This responds well to mobilization and stabilizing exercises.
A common problem area is the pelvis, low back and hip complex. Having skills in differential diagnosis is critical to differentiate a hip problem from a pelvis or low back problem. Clinically, it is very common that a patient has been told they have a hip problem when a thorough examination reveals a problem stemming from the low back. The lumbar spine sits on top of the pelvis, in particular the sacrum. The spine is like a chain with many small parts that should be mobile. In the lumbar spine the joints are formed to move sideways and forward and backward. This area is injured most often when bending forward, twisting and lifting. in our youth we see overtraining leading to injuries in particularly the low back. Education of coaches, parents and athletes is critical for recovery and return to sport. Tissues in the developing skeleton, particularly during a growth spurt, are weaker than in adults and prone to injury with excessive or repetitive forces. Once an injury is sustained, the risk for another injury increases dramatically as certain reflexive, protective core muscles associated with the injury are inactivated. Exercises that turn them on with out loading the injury are crucial to healing and reactivation of the core.
As we move up the spine to the thoracic spine, (or bröstryggen), the vertebrae are formed differently and move most easily sideways, forward and backward and in rotation. The ribs attach to the vertebrae (costovertebral joints) making up the chest and they attach in the front of the body to the sternum with the costosternal joints. The rib cage is susceptible to injury during heavy lifts and certain twisting movements. When the costovertebral joint is sprained, it can be difficult to take a deep breath or twist the upper body. This area is most commonly injured while lifting heavy things with outstretched arms. When the ribs are involved, the pain can travel around the rib and/or through the ribcage. Some people think they are having a heart or lung problem. Examination of this injury or dysfunction requires specialty education in biomechanics. We commonly treat this and show exercises which are necessary to stabilize the injured area.
The cervical spine (halsryggen) sits on top of the shoulders and bears the weight of the cranium. The cervical spine glides sideways, forward and backwards with the majority of rotation at the junction of the uppermost vertebrae and the cranium. The cervical spine is subject to injury with concussion adding to the symptom burden. The concussion symptoms sometimes overshadow the symptoms from the neck injury. Injuries to the neck which occurred previously can become symptomatic with excessive loading of the neck due to head posture in association with screen time. Pain in the shoulder, arm, elbow, wrist or hand can reflect a problem in the neck.
Neck pain can provoke of headaches in some individuals and addressing biomechanical issues in the neck can be an important part of the puzzle in resolving recurrent headaches. Headache and/or Neck Pain in Preadolescents: provoking factors
Recurrent headaches not uncommonly lead to a behavior where the jaw tightens and can complicate the headache symptom picture, why this is important to address. When parts of the “chain” or vertebrae are not moving as they should, there is a strain on the adjacent areas. The goal with treatment is to restore normal functioning and recommend exercises to make the area stable.
The shoulder complex is made up of the clavicle, the shoulder blade and the head of the humerus (top of the arm). The glenohumeral joint or the moveable part of the shoulder is rather unstable compared to the hip. It is more easily injured and requires very specific training to avoid common long-term problems. The clavicle and shoulder blade are less often injured, but may not function optimally with a shoulder injury. These are addressed in treatment and rehabilitation.
The elbow and wrist are common areas of complaint. The elbow is a unique joint which bends and can rotate. Depending on the type of injury or overuse syndrome which presents treatment addresses joint function and muscles that support the joint. The wrist has many small bones and the joints here must function perfectly to avoid pain and discomfort. In recent years complaints have increased with the monotone use of the arms at the computer. Good ergonomics are critical for avoiding overuse and appropriate information is an important aspect of rehabilitation.
Again, Pain in the shoulder, arm, elbow, wrist or hand can reflect a problem in the neck.
Our skills in differential diagnosis can determine where the problem comes from, whether it is a problem amenable to chiropractic care, or whether another specialist should examine the patient.
Studying and Gaming at Home:
Far from all homes are set up for children to study or game with good ergonomics. Things to think about to avoid neck and back pain are good ergonomics and establishing routines. Starting with routines, find a place to do exercises which activate core stability and plan do do them as a break from work. There are several basic programs under Rehab Övningar. Schedule in regular walks, bike rides, trampoline or other outside activity, ideally in the forest and activate the core muscles which you have worked with on the floor. A perfect time to engage with your child is after school and work, taking time to be together during a walk. This promotes conversation and is an opportunity to understand what life is like for your child.
Now lets look at the study and gaming station. Ergonomi : Ideally you sit in a comfortable chair with the knees lower than the hips, feet resting on the floor or another surface. The height of the desk is dictated by having a 90 degree angle at the elbow with the lower arm resting and pivoting on the desk (when using the mouse). This releases tension from the shoulder and neck. Ideally the tangent board and screen are separate. This allows you to raise the screen to an appropriate height. The screen height should be at eye height or slightly lower if you use computer glasses. The goal is to avoid creeping into the screen and finding yourself with the head positioned forward to your shoulders. The weight of the head increases the stress on the neck with about 25 kilos. Try to sit up straight and activate the core muscles so you are not hanging on your back. Think of this as a training session.
Idrottare
En idrottare är allt från barn som lär sig en sport, ungdomar som tränar, vuxna som tävlar till vuxna och äldre som håller sig igång. Som ung är det viktig att träningen är anpassad efter ålder, att man varierar tränings form, att man inte specialisera sig i en sport innan 15 år och att man inte spelar med de som är äldre. Allt detta är för att minimera risken för skada. Tränare har inge särskilt kunskåp om vad som händer i kroppen när den växer. Allvarliga skador är lätt missade och för att vinna, skadorna är ofta försummade. Senaste forsking från Danmark visar tydligt att barn klarar sig bättre från allvarliga idrottsskador genom att inte specialisera sig för tidigt. Helst ska man träna olika sporter medan kroppen utvecklas. Manska inte träna för intensivt under växt spurt och ålders grupper ska inte blandas.
 |
 |
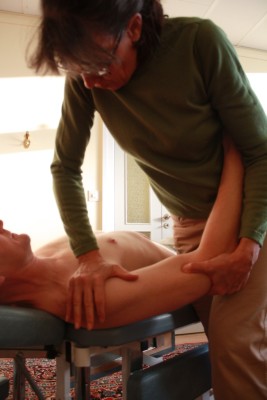 |
Behandling av den skadade idrottaren sker i flera steg. Först måste man ha kunskap för att diagnostisera problemet, vilket betyder att man måste förstå vad som är fel. Behandlingen har som mål att återställa funktionen, främja läkningen av den skadade vävnaden och sedan lära ut övningar som stabiliserar området. Stabilitet i bålen är grunden till balansen och kontroll i hela kroppen. Stabilitetsträning av bålen hör till träningen i alla åldersgrupper och alla sporter. För de som redan har haft nack- eller ryggbesvär är råd om lämplig träning viktig så man inte överanstränger det skadade området. Det är viktigt att titta på hela idrottaren. Förutom rygg eller nackbesvär är det vanligt med axel, arm, handled, höft, knä, fot eller ljumsksmärta hos idrottare. Det är viktigt att titta på hela individen och inte bara symtom området. Vid knä besvär eller lårmuskelproblem är det även viktigt att titta på bäcken, höft o ländrygg, (se nedan). När hela kroppen fungerar optimalt, kan man prestera maximalt. Råd om kost och näring är viktig för alla som tränar flera gånger i veckan.
World Spine Day 16/10
stresses the importance of self-help for back pain
World Spine Day is organized by the World Federation of Chiropractic on behalf of the Global Alliance for Musculoskeletal Health and this year highlights the global burden of spinal pain and disability. Low back pain is the biggest single global cause of years lived with disability. Chiropractic care has been shown to be effective in treating acute and chronic back pain with maintenance care reducing recurrent episodes of low back pain. Read more here
Guidelines for Treatment of Low Back Pain
The American College of Physicians (ACP) has presented guidelines for the treatment of low back pain based on the scientific evidence and provides clinical recommendations on noninvasive treatment of low back pain. The recommendations for all physicians treating patients with low back pain, whether acute or chronic conditions, was to avoid prescription of pharmacological agents and instead recommend spinal manipulation. For patients with chronic low back pain, besides spinal manipulation, other non-pharmacological recommendations are appropriate: exercise training to activate the core muscles; acupuncture; mindfulness; and relaxation techniques among others. As a chiropractic physician, treatment of low back pain varies depending on the diagnosis. Critical to all patients is learning what is neutral posture, how to activate the core to support it and then appropriate exercises to slowly strengthen the core without straining the back. Core training link. Techniques vary and include deep soft tissue, gentle mobilizing, activator technique (an instrument used apply a graded force to a joint, particularly when low force techniques are indicated) and manipulative joint techniques appropriate to the patients size and condition.
FÖREBYGGANDE BEHANDLING MINSKAR LÄNDRYGGSBESVÄR
Patienter som kom regelbundet till Kiropraktorn i förebyggande syftet under 12 månader hade mycket mindre besvär än patienter som kom när de hade besvär (Eklund, 2018).
Under 2010 har ledare i neurologi, medicin och forskare i kiropraktik samlat ihop vetenskaplig bevis angående kiropraktik även kallat manuell medicin och hur effektiv den är. De har funnit att efter de högsta kraven när det gäller vetenskapliga bevis kan man nu säga att kiropraktisk behandling med manipulation/mobilisering är effektiv behandling för:
- ont i ländryggen, båda den akuta och mer kroniska fasen av besvär
- migrän och huvudvärk som kommer från nacken
- yrsel som orsakas av nacken
- ont i nacke, båda den akuta och mer kroniska fasen av besvär. Nya bevis inom vetenskaplig forskning.
- problem med leder i armar och ben (axel, armbåge, handled samt höft, knä, vrist och fot)
- plantar fascit, carpal tunnel syndrom, rotator cuff syndrom
Rapporten visar att det finns positiva bevis för behandling av en del andra problem än rygg o nacke, både det som gäller övrig muskulatur och leder men också andra besvär .
Stukad vrist, ont i svanskotan, ischias, käkleds besvär (TMJ), spänningshuvudvärk samt PMS, mensvärk och lunginflammation hos äldre. Patienter som svarar positivt på behandling har ett problem med funktionen i lederna, och symptomen lindras när man återställer funktionen i de drabbade leder. Det finns även indikation att behandling kan vara effektivt vid astmabesvär.
Rapporten visar att behandling är både ofarlig och lämplig för alla ovan nämnda problem.
Utan tvekan kan man nu säga att manipulation/mobilisering utförd av kiropraktorer med utländsk godkänd utbildning (se www.LKR.se för svenskar med lämplig utbildning) är viktig i behandling av rygg och nackbesvär samt ont i huvudet.
Studier bekräftar vad vi har sett i praktiken sedan länge. Behandling av patienten i sin helhet förbättrar kroppens funktion och förmåga. Normal funktion of knä och höfter gör att ländryggen fungerar optimalt. När man börjar förlora rörlighet i de leder, sliter man på ländryggen och skynda de degenerativa förändringarna. Behandling av knä och höft problem så att de inte förlorar sin rörlighet minskar risken för ländryggs besvär.
Ergonomics at home and in the work place
Here is a group of pictures showing good ergonomics at home and in school. The basic principles are to vary standing and sitting. Standing is better for you body as long as it feels good. The screen should be at eye height until you use progressive eyeglasses, when the screen is slightly lowered. Avoid tilting your head to look at a screen. This protects your neck. The angle at the elbow should be 90 degrees and the lower arm resting and pivoting on the desk. This relieves shoulder and neck tension. Depending on the angle of the spine, it can be comfortable to have one foot on a stool, stand wide based with good posture.
For more information and pictures follow the link Ergonomi
Referenser:
Eklund A, Jensen I, Lohela-Karlsson M, Hagberg J, Leboeuf-Yde C. 2018. The Nordic Maintenance Care program: Effectiveness of chiropractic maintenance care versus symptom-guided treatment for recurrent and persistent low back pain—A pragmatic randomized controlled trial. PLoS ONE 13(9): e0203029. https://doi.org/10.1371/journal.pone.0203029
Qaseem A, Wilt T, McLean R, ForcieM. 2017. Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline From the American College of Physicians. Annals of internal medicine; 166(7):514-530.
Gross A, Langevin P, Burnie SJ, Bédard-Brochu MS, Empey B, Dugas E, Faber-Dobrescu M, Andres C, Graham N, Goldsmith CH, Brønfort G, Hoving JL, LeBlanc F. 2015. Manipulation and mobilisation for neck pain contrasted against an inactive control or another active treatment. Cochrane Database Syst Rev.;9:CD004249. doi: 10.1002/14651858.CD004249.pub4.
Clar C, Tsertsvadze A, Court R, Hundt GL, Clarke A, Sutcliffe P. 2014. Clinical effectiveness of manual therapy for the management of musculoskeletal and non-musculoskeletal conditions: systematic review and update of UK evidence report. Chiropr Man Therap;22(1):12. doi: 10.1186/2045-709X-22-12.
Bronfort G, Haas M et al. (2010). Effectiveness of manual therapies: The UK evidence report. Chiropractic & Osteopathy.18:3. Doi:10.1186/174601340018-3.
Haldeman S, Underwood M. (2010). Commentary on the United Kingdom Evidence Report about the effectiveness of manual therapies. Chiropractic & Osteopathy.18:4. Doi:10.1186/174601340018-4.
Hondras MA, Long CR, et al. (2009). A randomized controlled trial comparing 2 types of spinal manipulation and minimal conservative medical care for adults 55 years and older with subacute or chronic low-back pain. JMPT;32:330-43.
Senna MK, Machaly SA (2011) Does Maintained Spinal Manipulation Therapy for Chronic Non-Specific Low-Back Pain Result in Better Long Term Outcome? Spine DOI: 10.1097/BRS.0b013e3181f5dfe0.
Haldeman S, Chapman-Smith DA, Peterson DM eds (1993) Guidelines for Chiropractic Quality Assurance and Practice Parameters. Aspen Publishers, Gaithersburg, MD.
Henderson D, Chapman-Smith DA, Mior S, Vernon H eds (1994) Clinical Guidelines for Chiropractic Practice in Canada Suppl to JCCA 38(1).
Bigos S, Bowyer O, Braen G et al. (1994) Acute Low-Back Problems in Adults. Clinical Practice Guidelines No. 14. Rockville, Maryland: Agency for Health Care Policy and Research, Public Health Service, US Department of Health and Human Services AHC PR Publication No. 95-0642.
Murata Y, Takahashi K, Yamagata M, Hanaoka E, Moriya H. 2003. The knee-spine syndrome: Association between lumbar lordosis and extension of the knee; J Bone Joint Surg [Br];85-B:95-9.
Offierski CM, Macnab I. 1983. Hip-spine syndrome. Spine;8:316-21.
Chaibi , Russel M, Tuchin P. 2011. Manual therapies for migraine: a systematic review. J Headache Pain;12:127–133.